Posted by: Evelyn R
Post-traumatic stress disorder, or PTSD as it is commonly known, is a psychiatric disorder that can develop after a person experiences or is exposed to a traumatic event. Anyone can develop PTSD at any age, but not everyone that is faced with trauma will develop it; in fact, most people who experience trauma do not exhibit signs of the disorder. It is unclear why some individuals develop PTSD while others do not seem to experience any symptoms. Even though there are several aspects of PTSD that are unpredictable, including who develops which symptoms and why, two things are certain: treatment options are available, and there is hope for recovery.
What is trauma and where does it come from?
Trauma can be defined as “an experience that produces psychological injury or pain,” or that causes mental and/or emotional discomfort.1
Trauma can be experienced several different ways, which include:
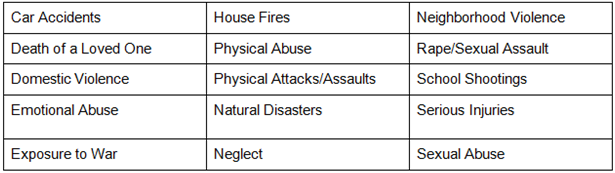
Some examples of traumatic events include:
Post-traumatic stress disorder, or PTSD as it is commonly known, is a psychiatric disorder that can develop after a person experiences or is exposed to a traumatic event. Anyone can develop PTSD at any age, but not everyone that is faced with trauma will develop it; in fact, most people who experience trauma do not exhibit signs of the disorder. It is unclear why some individuals develop PTSD while others do not seem to experience any symptoms. Even though there are several aspects of PTSD that are unpredictable, including who develops which symptoms and why, two things are certain: treatment options are available, and there is hope for recovery.
What is trauma and where does it come from?
Trauma can be defined as “an experience that produces psychological injury or pain,” or that causes mental and/or emotional discomfort.1
Trauma can be experienced several different ways, which include:
- Directly experiencing trauma (i.e. victimization of abuse or an attack)
- Witnessing a traumatic event in person (i.e. seeing a car crash)
- Finding out that a family member or close friend experienced a traumatic event
- Having repeated exposure to upsetting details of a traumatic event (i.e. emergency responders)2
Some examples of traumatic events include:
Symptoms of PTSD
Post-traumatic stress symptoms can appear immediately following a traumatic event or they may not appear until more than 6 months after the event, if at all; however, if someone is going to develop symptoms related to the trauma, it will usually happen within 3 months of when the trauma occurred. In order for someone to be diagnosed with PTSD, their symptoms must have a significantly negative impact on their ability to manage daily life. There are 4 categories of symptoms used to diagnose PTSD:
Some commonly known re-experiencing symptoms of PTSD include nightmares, flashbacks, and intrusive thoughts related to the traumatic event(s). Reminders of the trauma that cause a person to feel emotional distress and/or to experience physical symptoms, such as sweating or a pounding heart, are other possible symptoms.3
Avoidance symptoms consist of avoiding thoughts and feelings related to the trauma, and/or avoiding physical reminders of the trauma including people, places, activities, or objects. There are various ways that an individual may exhibit avoidance; some people might refuse to mention or talk about the trauma, some might become more withdrawn from friends and family members, and some people may pretend that the trauma never happened.3
Arousal/Reactivity symptoms pertain to how alert and responsive a person is to what is happening in their mind and body, as well as to what is going on around them. Increased irritability or angry outbursts following a traumatic event are common symptoms in this category. Negative changes in sleep patterns or ability to concentrate are also possible, as well as startling more easily, feeling “on edge” or constantly looking for signs of trouble, and engaging in dangerous or self-destructive behavior.4
Mood and cognitive symptoms have a negative impact on the individual’s emotions and thoughts. After a traumatic experience, some people have a hard time remembering parts of what happened. Many people who develop PTSD feel extremely guilty or shameful about the event, even if it was out of their control, and many people also report having inaccurate thoughts about themselves (i.e. “I am a bad person”) or about the world (i.e. “No one is trustworthy”). Additionally, some individuals begin experiencing negative emotions more frequently, and it may become increasingly difficult for them to feel positive emotions. Trauma survivors sometimes lose interest in activities that are usually enjoyable, and they may find themselves feeling more distant or detached from the people closest to them.4
Children with PTSD
Children diagnosed with PTSD experience many of the same symptoms as adults but, due to their age and developmental level, their symptoms are often expressed differently. Children may repeatedly reenact the traumatic event in their play, or they may begin to show less interest in their usual activities and spend less time engaged in play. Some children may become insistent on staying by their parent or caregiver’s side, and show distress when faced with separation from that person. Some children with PTSD may revert to behavior from an earlier stage of development, such as wetting the bed or forgetting how to speak. Other children may start acting out more with disruptive or destructive behaviors along with disrespect for the people around them.2
PTSD and Other Symptoms
It is not uncommon for individuals with PTSD to have other mental or physical health concerns. Some people who have been diagnosed with post-traumatic stress disorder may have additional anxiety- or depression-related symptoms. There are some trauma survivors who experience challenges in maintaining relationships with friends or family, and some people may use drugs and/or alcohol to cope with the effects of trauma. Some individuals report having persistent physical symptoms stemming from the trauma such as headaches, stomachaches, or back pain. Thoughts of suicide are another potential symptom that may arise after experiencing trauma. Suicidal ideation should always be taken seriously; if you or someone you know is thinking about suicide, please call the National Suicide Prevention Hotline at 1-800-237-TALK (8255).3
Some trauma survivors may experience only 1 or 2 symptoms of post-traumatic stress, while others report having multiple symptoms; symptoms may persist for several months or they may last only days or weeks. There are also some people who may not develop any symptoms. Everyone reacts differently to traumatic experiences, and there is no “right” or “wrong” way to respond. Regardless of how you or a family member or friend might experience trauma-related symptoms, it is normal to be faced with challenges in coping and recovering from the trauma.
Risk/Resilience Factors
Researchers have yet to determine why some people develop PTSD while others do not. Despite this lack of understanding, some factors that may influence whether a person will present with trauma-related symptoms have been identified. Risk factors may increase a person’s chance of developing PTSD, but the presence of any risk factors does not mean that they will develop disorder. Resilience factors are believed to help protect a person from the negative effects of trauma, but their presence does not mean that the individual is immune from post-traumatic disorder.2
Some risk factors include: (1) childhood trauma, (2) having little/no support after the traumatic event, (3) seeing someone get hurt or die, and (4) history of mental illness.2
Some resilience factors include: (1) support from friends/family, (2) utilizing positive coping skills, (3) presence of self-esteem, and (4) having hope for the future.2
Treatment Options & Self-Care
Not everyone with trauma-related symptoms will need treatment to achieve recovery, but many do need that extra support. Treatment options for PTSD include medication, talk therapy (counseling), and alternative therapies. Some trauma survivors choose to ask their doctor for a prescription to help manage their symptoms. In some cases, a person may choose to take a medication, such as an antidepressant, for an extended period so that they can function in their day-to-day life. Other individuals may choose to take a medication just for the duration of talk therapy, because the medicine can help reduce their symptoms allowing them to place more focus on learning new skills and getting as much out of the counseling experience as possible.1,2
There are some individuals who to attend talk therapy sessions as their sole form of treatment. Cognitive behavioral therapy is one of the most commonly used types of talk therapy, and its purpose is to help individuals process the thoughts and feelings related to the trauma in a way that will allow them to create a more positive perception of the traumatic event(s). Talk therapy can be utilized in individual and groups sessions, and it usually lasts 6-12 weeks, but may extend beyond that depending on the person’s needs. Alternative therapies, such as acupuncture and animal-assisted therapy, are also available, but information regarding the effectiveness of these less conventional therapies is still quite limited.1,2
Taking care of oneself is always important, but it becomes especially critical when faced with a traumatic experience. Self-care involves setting aside time for relaxing and using healthy coping skills to manage stress. Self-care is different for everyone, but one key aspect of it is to be patient with oneself while recovering from trauma. Self-care activities may include, but are not limited to writing in a journal, listening to music, engaging in physical activity, making time to get enough sleep, eating well, and attending a PTSD support group.1,2
Post-traumatic stress symptoms can appear immediately following a traumatic event or they may not appear until more than 6 months after the event, if at all; however, if someone is going to develop symptoms related to the trauma, it will usually happen within 3 months of when the trauma occurred. In order for someone to be diagnosed with PTSD, their symptoms must have a significantly negative impact on their ability to manage daily life. There are 4 categories of symptoms used to diagnose PTSD:
- Re-experiencing symptoms
- Avoidance symptoms
- Arousal/Reactivity symptoms
- Mood and Cognitive symptoms2
Some commonly known re-experiencing symptoms of PTSD include nightmares, flashbacks, and intrusive thoughts related to the traumatic event(s). Reminders of the trauma that cause a person to feel emotional distress and/or to experience physical symptoms, such as sweating or a pounding heart, are other possible symptoms.3
Avoidance symptoms consist of avoiding thoughts and feelings related to the trauma, and/or avoiding physical reminders of the trauma including people, places, activities, or objects. There are various ways that an individual may exhibit avoidance; some people might refuse to mention or talk about the trauma, some might become more withdrawn from friends and family members, and some people may pretend that the trauma never happened.3
Arousal/Reactivity symptoms pertain to how alert and responsive a person is to what is happening in their mind and body, as well as to what is going on around them. Increased irritability or angry outbursts following a traumatic event are common symptoms in this category. Negative changes in sleep patterns or ability to concentrate are also possible, as well as startling more easily, feeling “on edge” or constantly looking for signs of trouble, and engaging in dangerous or self-destructive behavior.4
Mood and cognitive symptoms have a negative impact on the individual’s emotions and thoughts. After a traumatic experience, some people have a hard time remembering parts of what happened. Many people who develop PTSD feel extremely guilty or shameful about the event, even if it was out of their control, and many people also report having inaccurate thoughts about themselves (i.e. “I am a bad person”) or about the world (i.e. “No one is trustworthy”). Additionally, some individuals begin experiencing negative emotions more frequently, and it may become increasingly difficult for them to feel positive emotions. Trauma survivors sometimes lose interest in activities that are usually enjoyable, and they may find themselves feeling more distant or detached from the people closest to them.4
Children with PTSD
Children diagnosed with PTSD experience many of the same symptoms as adults but, due to their age and developmental level, their symptoms are often expressed differently. Children may repeatedly reenact the traumatic event in their play, or they may begin to show less interest in their usual activities and spend less time engaged in play. Some children may become insistent on staying by their parent or caregiver’s side, and show distress when faced with separation from that person. Some children with PTSD may revert to behavior from an earlier stage of development, such as wetting the bed or forgetting how to speak. Other children may start acting out more with disruptive or destructive behaviors along with disrespect for the people around them.2
PTSD and Other Symptoms
It is not uncommon for individuals with PTSD to have other mental or physical health concerns. Some people who have been diagnosed with post-traumatic stress disorder may have additional anxiety- or depression-related symptoms. There are some trauma survivors who experience challenges in maintaining relationships with friends or family, and some people may use drugs and/or alcohol to cope with the effects of trauma. Some individuals report having persistent physical symptoms stemming from the trauma such as headaches, stomachaches, or back pain. Thoughts of suicide are another potential symptom that may arise after experiencing trauma. Suicidal ideation should always be taken seriously; if you or someone you know is thinking about suicide, please call the National Suicide Prevention Hotline at 1-800-237-TALK (8255).3
Some trauma survivors may experience only 1 or 2 symptoms of post-traumatic stress, while others report having multiple symptoms; symptoms may persist for several months or they may last only days or weeks. There are also some people who may not develop any symptoms. Everyone reacts differently to traumatic experiences, and there is no “right” or “wrong” way to respond. Regardless of how you or a family member or friend might experience trauma-related symptoms, it is normal to be faced with challenges in coping and recovering from the trauma.
Risk/Resilience Factors
Researchers have yet to determine why some people develop PTSD while others do not. Despite this lack of understanding, some factors that may influence whether a person will present with trauma-related symptoms have been identified. Risk factors may increase a person’s chance of developing PTSD, but the presence of any risk factors does not mean that they will develop disorder. Resilience factors are believed to help protect a person from the negative effects of trauma, but their presence does not mean that the individual is immune from post-traumatic disorder.2
Some risk factors include: (1) childhood trauma, (2) having little/no support after the traumatic event, (3) seeing someone get hurt or die, and (4) history of mental illness.2
Some resilience factors include: (1) support from friends/family, (2) utilizing positive coping skills, (3) presence of self-esteem, and (4) having hope for the future.2
Treatment Options & Self-Care
Not everyone with trauma-related symptoms will need treatment to achieve recovery, but many do need that extra support. Treatment options for PTSD include medication, talk therapy (counseling), and alternative therapies. Some trauma survivors choose to ask their doctor for a prescription to help manage their symptoms. In some cases, a person may choose to take a medication, such as an antidepressant, for an extended period so that they can function in their day-to-day life. Other individuals may choose to take a medication just for the duration of talk therapy, because the medicine can help reduce their symptoms allowing them to place more focus on learning new skills and getting as much out of the counseling experience as possible.1,2
There are some individuals who to attend talk therapy sessions as their sole form of treatment. Cognitive behavioral therapy is one of the most commonly used types of talk therapy, and its purpose is to help individuals process the thoughts and feelings related to the trauma in a way that will allow them to create a more positive perception of the traumatic event(s). Talk therapy can be utilized in individual and groups sessions, and it usually lasts 6-12 weeks, but may extend beyond that depending on the person’s needs. Alternative therapies, such as acupuncture and animal-assisted therapy, are also available, but information regarding the effectiveness of these less conventional therapies is still quite limited.1,2
Taking care of oneself is always important, but it becomes especially critical when faced with a traumatic experience. Self-care involves setting aside time for relaxing and using healthy coping skills to manage stress. Self-care is different for everyone, but one key aspect of it is to be patient with oneself while recovering from trauma. Self-care activities may include, but are not limited to writing in a journal, listening to music, engaging in physical activity, making time to get enough sleep, eating well, and attending a PTSD support group.1,2
Resources
National Institute of Mental Health - About PTSD https://www.nimh.nih.gov/health/topics/post-traumatic-stress-disorder-ptsd/index.shtml
Help Guide - About PTSD, Treatment, & Finding Therapy
http://www.helpguide.org/articles/ptsd-trauma/post-traumatic-stress-disorder.htm
KidsHealth - PTSD - For Parents
http://kidshealth.org/en/parents/ptsd.html
TeensHealth - PTSD - For Teens
http://kidshealth.org/en/teens/ptsd.html?ref=search
National Suicide Prevention Lifeline: 1-800-237-TALK (8255)
http://suicidepreventionlifeline.org/
References
1 "The Definition of Trauma." Dictionary.com. Random House, Inc., 2016. Web. 31 Oct. 2016.
2 "NIMH » Post-Traumatic Stress Disorder." National Institute of Mental Health. U.S. National Library of Medicine, 2016. Web. 31 Oct. 2016.
3"Post-Traumatic Stress Disorder." Mental Health America. Mental Health America, 2016. Web. 31 Oct. 2016.
4"What Is Posttraumatic Stress Disorder?" What Is PTSD? American Psychiatric Association, 2016. Web. 31 Oct. 2016.
National Institute of Mental Health - About PTSD https://www.nimh.nih.gov/health/topics/post-traumatic-stress-disorder-ptsd/index.shtml
Help Guide - About PTSD, Treatment, & Finding Therapy
http://www.helpguide.org/articles/ptsd-trauma/post-traumatic-stress-disorder.htm
KidsHealth - PTSD - For Parents
http://kidshealth.org/en/parents/ptsd.html
TeensHealth - PTSD - For Teens
http://kidshealth.org/en/teens/ptsd.html?ref=search
National Suicide Prevention Lifeline: 1-800-237-TALK (8255)
http://suicidepreventionlifeline.org/
References
1 "The Definition of Trauma." Dictionary.com. Random House, Inc., 2016. Web. 31 Oct. 2016.
2 "NIMH » Post-Traumatic Stress Disorder." National Institute of Mental Health. U.S. National Library of Medicine, 2016. Web. 31 Oct. 2016.
3"Post-Traumatic Stress Disorder." Mental Health America. Mental Health America, 2016. Web. 31 Oct. 2016.
4"What Is Posttraumatic Stress Disorder?" What Is PTSD? American Psychiatric Association, 2016. Web. 31 Oct. 2016.
 RSS Feed
RSS Feed
